Autism Around the World: How Different Countries Approach Diagnosis
The global landscape of autism diagnosis is as diverse as the cultures and healthcare systems that shape it. From the meticulous screening protocols of Nordic nations to the emerging frameworks in parts of Africa and Asia, the methodologies employed to identify autism spectrum disorder (ASD) reflect a tapestry of medical, social, and technological advancements. This variability underscores not only the complexity of neurodevelopmental conditions but also the evolving understanding of how best to recognize and support individuals across different societal contexts. Understanding these approaches offers a lens into the broader challenges of healthcare equity, cultural perceptions, and the intersection of policy with clinical practice.
Diagnostic frameworks are not merely clinical tools; they are cultural artifacts that reveal how societies perceive neurodiversity. In some regions, early and intensive screening has become a cornerstone of public health initiatives, while in others, diagnostic pathways remain fragmented, hindered by stigma or limited resources. The methodologies range from standardized questionnaires administered in pediatric clinics to community-based screenings in rural areas, each tailored to the unique needs and constraints of the population. This article explores the multifaceted approaches to autism diagnosis worldwide, examining the systems, innovations, and challenges that define this critical first step in the journey of support and inclusion.
The Nordic Model: Precision and Early Intervention
Scandinavian countries, particularly Sweden and Denmark, have long been at the vanguard of autism diagnosis, characterized by a blend of universal healthcare access and rigorous developmental surveillance. Their systems prioritize early detection through a combination of mandatory well-child visits and parent-report screening tools such as the Modified Checklist for Autism in Toddlers (M-CHAT). These screenings are often integrated into routine pediatric care, ensuring that even subtle developmental deviations are flagged before they escalate into more pronounced challenges.
The Nordic approach is distinguished by its longitudinal tracking of developmental milestones, with data from prenatal visits through adolescence feeding into a centralized health registry. This longitudinal perspective enables clinicians to identify not only overt signs of ASD but also subtle precursors, such as delayed joint attention or atypical sensory processing. Additionally, the region’s emphasis on multidisciplinary teams—comprising pediatricians, child psychologists, and speech therapists—ensures that diagnoses are not rendered in isolation but are instead the product of comprehensive, consensus-driven evaluations.
Another hallmark of the Nordic model is its integration of digital tools. Telemedicine platforms facilitate remote consultations, particularly in remote or sparsely populated areas, while AI-driven screening algorithms analyze developmental data to flag potential cases for further review. This technological integration reflects a broader trend toward precision medicine, where data analytics and clinical intuition converge to refine diagnostic accuracy. The result is a system that not only identifies autism early but also tailors interventions to the individual’s developmental profile, setting the stage for more effective support.

The Anglo-American Paradigm: Surveillance and Standardization
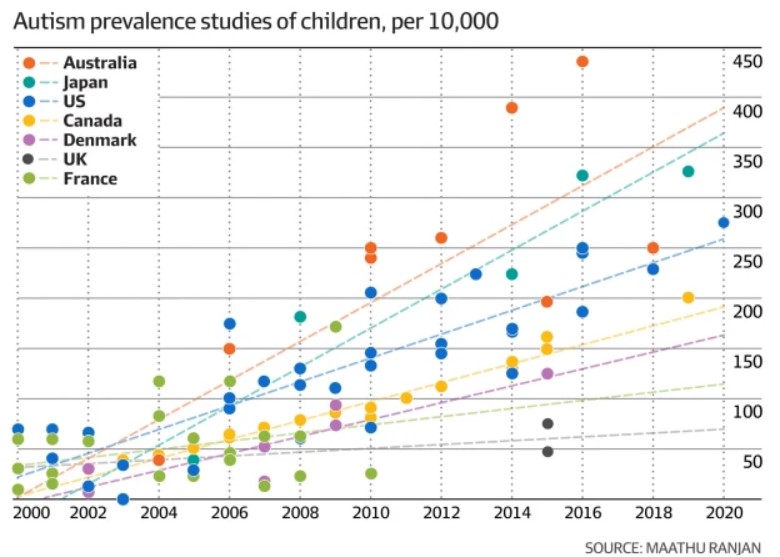
The United States and the United Kingdom have developed distinct yet interconnected approaches to autism diagnosis, both rooted in large-scale epidemiological surveillance and standardized diagnostic criteria. In the U.S., the Centers for Disease Control and Prevention (CDC) conducts biennial surveys, such as the Autism and Developmental Disabilities Monitoring (ADDM) Network, which aggregates data from multiple communities to estimate prevalence rates. These surveys rely on retrospective reviews of medical and educational records, providing a population-level snapshot of autism trends over time.
The American diagnostic process is heavily influenced by the Diagnostic and Statistical Manual of Mental Disorders (DSM-5), which outlines specific criteria for ASD, including impairments in social communication and restricted, repetitive behaviors. Clinicians typically employ a combination of the Autism Diagnostic Observation Schedule (ADOS-2) and the Autism Diagnostic Interview-Revised (ADI-R) to confirm diagnoses, tools that have been meticulously validated across diverse populations. However, the reliance on these standardized instruments has sparked debates about cultural bias, as some argue that the criteria may not fully capture the nuances of autism presentation in non-Western contexts.
In the UK, the National Institute for Health and Care Excellence (NICE) guidelines emphasize a staged approach to diagnosis, beginning with universal developmental checks at 18 and 24 months, followed by referrals to specialist autism teams if concerns arise. The system is designed to balance early detection with the avoidance of overdiagnosis, a challenge exacerbated by the growing awareness of autism in recent decades. The UK’s approach also places significant emphasis on the role of general practitioners (GPs) as gatekeepers, a model that has both strengths and limitations. While GPs are well-positioned to identify early red flags, their limited training in neurodevelopmental disorders can lead to delays or misdiagnoses, particularly in cases where autism co-occurs with other conditions such as ADHD or anxiety.
Eastern Innovations: Cultural Adaptations and Community Engagement
In East Asia, countries like Japan, South Korea, and China have developed diagnostic frameworks that reflect both technological advancements and deep-rooted cultural attitudes toward neurodiversity. Japan, for instance, has pioneered the use of school-based screening programs, where teachers and school nurses play a pivotal role in identifying children who may require further evaluation. This approach leverages the close-knit nature of Japanese educational institutions, where professionals are often attuned to subtle behavioral differences in students. However, the system is not without its challenges, as the stigma associated with mental health conditions in Japan can deter families from pursuing formal diagnoses, leading to underreporting in official statistics.
South Korea has taken a more centralized approach, with the government implementing nationwide autism screening programs that target infants and toddlers. The country’s National Autism Registry, established in 2016, serves as a comprehensive database for tracking diagnosed cases, enabling policymakers to allocate resources more effectively. The registry also facilitates research into the genetic and environmental factors contributing to autism, positioning South Korea as a leader in data-driven public health initiatives. Yet, the registry’s existence has raised privacy concerns, highlighting the delicate balance between surveillance and individual autonomy.
In China, the diagnostic landscape is rapidly evolving, with urban centers like Beijing and Shanghai adopting Western-style assessment tools while rural areas lag behind due to limited access to trained professionals. The Chinese government has begun to address these disparities through initiatives such as the “Sunshine Project,” which aims to train community workers in basic autism recognition and provide telemedicine consultations in underserved regions. These efforts are gradually bridging the urban-rural divide, though cultural beliefs—such as the historical preference for attributing developmental delays to “laziness” or “poor parenting”—continue to pose barriers to early diagnosis.
The Global South: Emerging Frameworks and Persistent Gaps
In many parts of Africa, Latin America, and South Asia, the diagnostic landscape for autism is characterized by fragmentation and resource constraints. In India, for example, the lack of standardized screening protocols has led to significant delays in diagnosis, with many children only being identified after they enter school and struggle to meet academic or social expectations. Non-governmental organizations (NGOs) have stepped into this void, establishing community-based screening programs that rely on parent training and culturally adapted assessment tools. These grassroots initiatives often serve as the first line of defense against diagnostic neglect, though their reach remains limited by funding and logistical challenges.
In sub-Saharan Africa, autism diagnosis is further complicated by the absence of culturally relevant assessment tools. Many standardized questionnaires, such as the M-CHAT, have not been validated for local languages or cultural contexts, leading to high rates of misdiagnosis or missed cases. Efforts to adapt these tools—such as the development of Swahili or Yoruba versions of screening instruments—are underway, but progress is slow. Additionally, the stigma surrounding neurodevelopmental disorders in many African communities can deter families from seeking help, perpetuating cycles of isolation and delayed intervention. Despite these challenges, countries like South Africa have made strides in integrating autism awareness into primary healthcare, with nurses receiving basic training in recognizing early signs during routine check-ups.
Latin America presents a mixed picture, with countries like Argentina and Brazil leading the way in public health initiatives, while others grapple with systemic inequities. Argentina’s “Autism Law,” enacted in 2014, mandates early diagnosis and intervention, though implementation varies widely across provinces. In Brazil, the government has invested in training programs for healthcare workers, particularly in the Amazon region, where access to specialists is scarce. However, economic instability and political turmoil in some Latin American nations have stymied progress, leaving many families to navigate the diagnostic maze without institutional support.
The Future of Global Autism Diagnosis: Toward Equity and Innovation
The trajectory of autism diagnosis worldwide is being shaped by two powerful forces: technological innovation and the growing recognition of neurodiversity as a global human rights issue. Artificial intelligence, for instance, is poised to revolutionize early detection, with machine learning algorithms capable of analyzing home videos or wearable sensor data to identify potential red flags in real time. These tools could democratize access to screening, particularly in regions where trained professionals are scarce, though ethical concerns about data privacy and algorithmic bias must be carefully addressed.
Another transformative trend is the shift toward participatory models of diagnosis, where families and autistic individuals themselves play an active role in the process. Community-led initiatives, such as peer support groups and self-advocacy networks, are challenging the traditional medical model of autism, advocating instead for a strengths-based approach that emphasizes individual needs and preferences. This paradigm shift is particularly evident in countries like Canada and Australia, where autistic-led organizations are influencing policy and practice, ensuring that diagnostic frameworks are not only accurate but also respectful of neurodivergent identities.
Yet, the path forward is not without obstacles. The COVID-19 pandemic exposed and exacerbated existing disparities in autism diagnosis, with lockdowns and healthcare disruptions leading to significant backlogs in assessments. The pandemic also highlighted the resilience of telemedicine, which emerged as a critical tool for maintaining continuity of care in regions where in-person evaluations were impossible. As the world emerges from the pandemic, the challenge will be to build on these innovations while addressing the systemic inequities that continue to marginalize autistic individuals in low-resource settings.
The journey toward equitable autism diagnosis is a testament to the power of collective action—one that demands collaboration across borders, disciplines, and communities. By learning from the successes and failures of diverse diagnostic frameworks, societies can forge a future where every individual, regardless of geography or background, has the opportunity to thrive. The road ahead is long, but the destination—a world where autism is understood, recognized, and supported on its own terms—is within reach.