In the labyrinth of the human mind, two enigmatic pathways diverge—one illuminated by the prism of autism, the other shrouded in the mist of schizophrenia. For decades, these conditions have been viewed through the narrow lens of misconception, their complexities reduced to caricatures of social withdrawal or erratic behavior. Yet, beneath the surface lies a tapestry of nuanced differences, woven from distinct neurobiological threads and divergent developmental trajectories. To conflate autism and schizophrenia is to mistake the brushstrokes of two masterpieces for a single, blurred canvas. This exploration seeks not merely to distinguish them but to illuminate the profound ways in which they diverge, challenging long-held assumptions and inviting a paradigm shift in how we perceive these conditions.
Consider the child who retreats into a world of repetitive rituals, their focus razor-sharp on the flicker of a spinning top, oblivious to the chatter around them. Now, contrast this with the adult whose thoughts spiral into paranoid delusions, their grip on reality slipping like sand through fingers. At first glance, both scenarios paint a picture of detachment, yet the essence of their experiences could not be more disparate. Autism and schizophrenia, though sometimes overlapping in their outward manifestations, are fundamentally distinct in their origins, developmental timelines, and cognitive signatures. To understand them is to unravel the intricate dance between neurodiversity and neurodivergence, where one reflects a lifelong neurobiological variance and the other a disruptive fracture in mental equilibrium.
The Genesis of Divergence: Developmental Roots and Onset
Autism, a neurodevelopmental condition, emerges in the crucible of early childhood, its roots embedded in the prenatal and perinatal stages of brain development. The neural pathways of an autistic individual often follow an atypical trajectory from the outset, characterized by differences in synaptic pruning, connectivity, and regional specialization. These differences manifest in early infancy—delayed babbling, aversion to eye contact, or an insatiable fixation on sensory stimuli—signals that the brain is wiring itself in a manner distinct from the neurotypical mold.
Schizophrenia, on the other hand, is a psychotic disorder that typically rears its head in late adolescence or early adulthood, a temporal divide that underscores its distinct nature. The onset of schizophrenia is often preceded by a prodromal phase, a liminal space where subtle cognitive and social deficits emerge, gradually crystallizing into the full-blown symptoms of hallucinations, delusions, and disorganized thinking. Unlike autism, which is present from birth, schizophrenia represents a deviation from an otherwise typical developmental path, a rupture in the continuity of mental function. This divergence in onset—one rooted in the cradle, the other in the crucible of young adulthood—hints at the fundamentally different mechanisms at play.
The distinction becomes even more pronounced when examining the role of genetics. Autism exhibits a strong hereditary component, with concordance rates in monozygotic twins approaching 70-90%, suggesting a polygenic inheritance pattern. In contrast, schizophrenia’s genetic architecture is more complex, involving rare de novo mutations and a higher degree of environmental interplay, such as prenatal infections or obstetric complications. These genetic fingerprints not only differentiate the two conditions but also underscore their divergent etiologies.
Cognitive and Perceptual Landscapes: Where the Mind Wanders

To traverse the cognitive landscapes of autism and schizophrenia is to step into two radically different worlds. In autism, the mind often operates with an unparalleled intensity, hyperfocused on details while struggling to synthesize the broader context. This phenomenon, known as weak central coherence, explains why an autistic individual might memorize train schedules with ease yet struggle to grasp the emotional undertones of a conversation. The autistic brain is not broken; it is wired differently, prioritizing pattern recognition and literal interpretation over the fluid, inferential leaps that neurotypical cognition thrives on.
Schizophrenia, conversely, fractures the very fabric of reality. The hallmark symptoms—hallucinations and delusions—are not merely distortions of perception but active rewritings of the mind’s narrative. A voice that whispers commands, a belief that one’s thoughts are being broadcast to the world, or the conviction that one’s body is being manipulated by external forces—these are not misinterpretations but invasions of the self. The cognitive dissonance in schizophrenia is not a matter of detail-oriented thinking but a collapse of the boundaries between the internal and external worlds. Where autism’s cognitive style is one of hyper-specificity, schizophrenia’s is a descent into chaos, where the mind’s usual filters dissolve into noise.
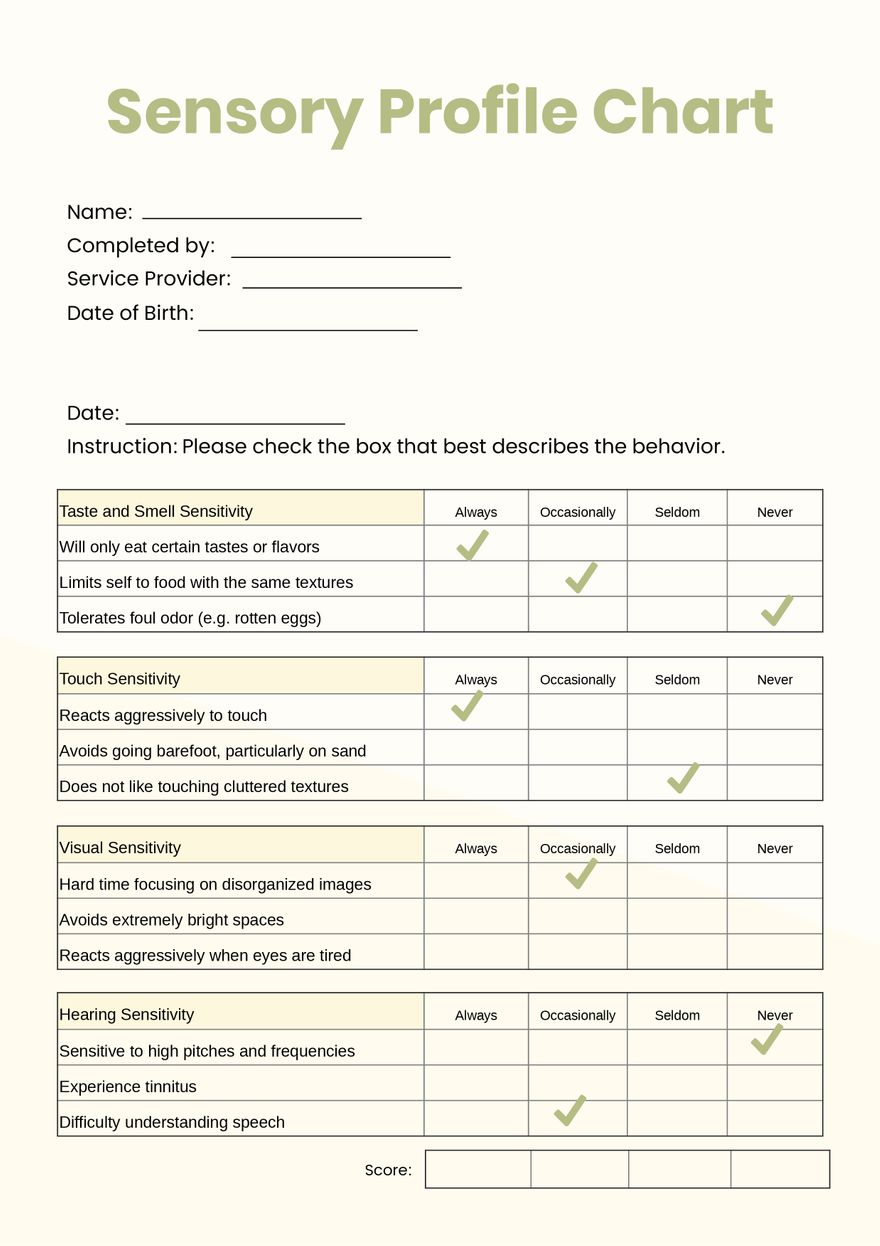
This perceptual divide extends to sensory experiences. Autistic individuals often report heightened sensitivity to stimuli—textures that feel like sandpaper, sounds that pierce like needles—yet these sensations are consistent and predictable within their own framework. In schizophrenia, sensory disturbances are more erratic, ranging from synesthesia-like blending of senses to the terrifying belief that one’s body is being controlled by an external entity. The autistic individual may seek to control their environment to mitigate sensory overload; the individual with schizophrenia may struggle to distinguish their own agency from the perceived manipulations of others.
Social Cognition: The Dance of Connection and Disconnection
Social interaction is the crucible in which the differences between autism and schizophrenia become most stark. Autistic individuals often experience a profound disconnect in their ability to read social cues, not out of a lack of desire for connection but due to a fundamental difference in how social information is processed. Theory of Mind—the ability to attribute mental states to others—is not absent in autism but is frequently delayed or qualitatively different. An autistic child might not instinctively understand sarcasm or recognize a friend’s distress, not because they are indifferent, but because their brain does not automatically map emotions onto facial expressions or tone of voice.
In schizophrenia, the breakdown in social cognition is more insidious, rooted in the erosion of trust and the fragmentation of identity. Paranoia and social withdrawal in schizophrenia are not merely the result of misreading cues but a defensive retreat from a world perceived as hostile or illusory. The individual with schizophrenia may avoid eye contact not out of disinterest but because they believe their gaze is being weaponized against them. Where autism’s social challenges stem from a different operating system, schizophrenia’s arise from a system that has been hijacked by delusional logic.
This distinction is further illuminated by the role of empathy. Autistic individuals often exhibit a form of empathy that is cognitively driven rather than emotionally intuitive—they may intellectualize another’s feelings but struggle to mirror them instinctively. In schizophrenia, empathy is not absent but distorted by the prism of paranoia; the individual may believe others are experiencing emotions that align with their delusions, creating a feedback loop of mistrust and isolation.
The Myth of Overlap: When Diagnoses Collide
Despite their differences, autism and schizophrenia are not mutually exclusive. A small subset of individuals may receive both diagnoses, a phenomenon that has fueled debates about shared etiological pathways. However, this overlap is more likely a reflection of diagnostic overshadowing—the tendency to attribute all symptoms to one condition while overlooking the other. For instance, an autistic individual experiencing severe anxiety might be misdiagnosed with schizophrenia due to their social withdrawal and erratic behavior, when in reality, their distress stems from sensory overload and the inability to communicate their needs.
Research into shared genetic risk factors, such as the *C4* gene associated with synaptic pruning, has suggested potential biological overlaps. Yet, these findings do not negate the fundamental differences between the conditions. Instead, they underscore the complexity of the human brain, where distinct pathways can converge on similar behavioral outcomes. The key lies in recognizing that even in cases of comorbidity, the core experiences of autism and schizophrenia remain distinct—one a lifelong neurodivergence, the other a episodic or chronic disruption of mental function.
Rethinking Support: Tailored Interventions for Distinct Needs
The implications of these differences extend far beyond academic debate; they shape the interventions and accommodations that can transform lives. For autistic individuals, support often revolves around creating structured environments, leveraging special interests as tools for engagement, and teaching adaptive social strategies. The goal is not to “normalize” behavior but to provide scaffolding that allows the individual to navigate a world not designed for their neurobiology.
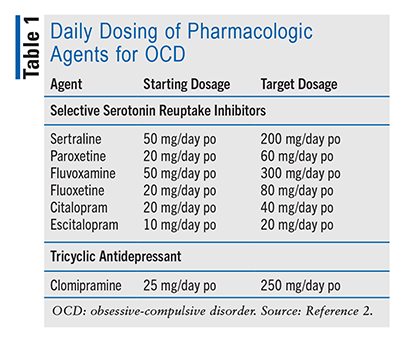
In schizophrenia, interventions focus on stabilizing reality through medication, cognitive-behavioral therapy, and social skills training designed to counteract delusional thinking. The emphasis is on restoring a sense of agency and coherence in a mind that has become fractured. Where autism requires a bridge between the individual and the world, schizophrenia demands a reconstruction of the self within that world.
This tailored approach is not merely a matter of semantics but a recognition of the profound differences in how these conditions manifest. An autistic individual may benefit from noise-canceling headphones to manage sensory overload; an individual with schizophrenia may require antipsychotic medication to quiet the voices that command their actions. The former seeks accommodation; the latter seeks restoration.

A New Perspective: Embracing Complexity Without Stigma
The journey to understanding autism and schizophrenia is not one of binary opposition but of nuanced distinction. To label them as variations of the same phenomenon is to flatten the richness of human cognition into a monochrome sketch. Instead, we must embrace a perspective that acknowledges their differences while remaining open to the intersections where they may overlap.
This shift in perspective is not merely academic; it has real-world consequences. It informs how we educate, how we diagnose, and how we support individuals navigating these conditions. It challenges the stigma that has long conflated neurodivergence with dysfunction, replacing it with a narrative of diversity—one where the autistic mind and the schizophrenic mind are not broken but different, each offering a unique lens through which to view the world.
As we peel back the layers of misconception, we uncover not just the differences between autism and schizophrenia but the broader truth about the human brain: it is a landscape of infinite variability, where no two minds are wired alike. To understand this is to take the first step toward a future where neurodiversity is not just accepted but celebrated, and where the pathways of the mind are no longer shrouded in mystery but illuminated by clarity.