Puberty is an intricate and profound period marked by significant hormonal upheaval and physiological transformation. For individuals on the autism spectrum, this transitional phase can pose unique challenges and nuances that intertwine neurodevelopmental characteristics with the biological tides of maturation. Understanding the interplay between autism and hormonal changes is crucial not only for caregivers and professionals but also for the individuals themselves, as they navigate a labyrinth of sensory, emotional, and behavioral shifts that puberty and the years beyond entail.
Hormonal Foundations of Puberty: A Complex Biological Symphony
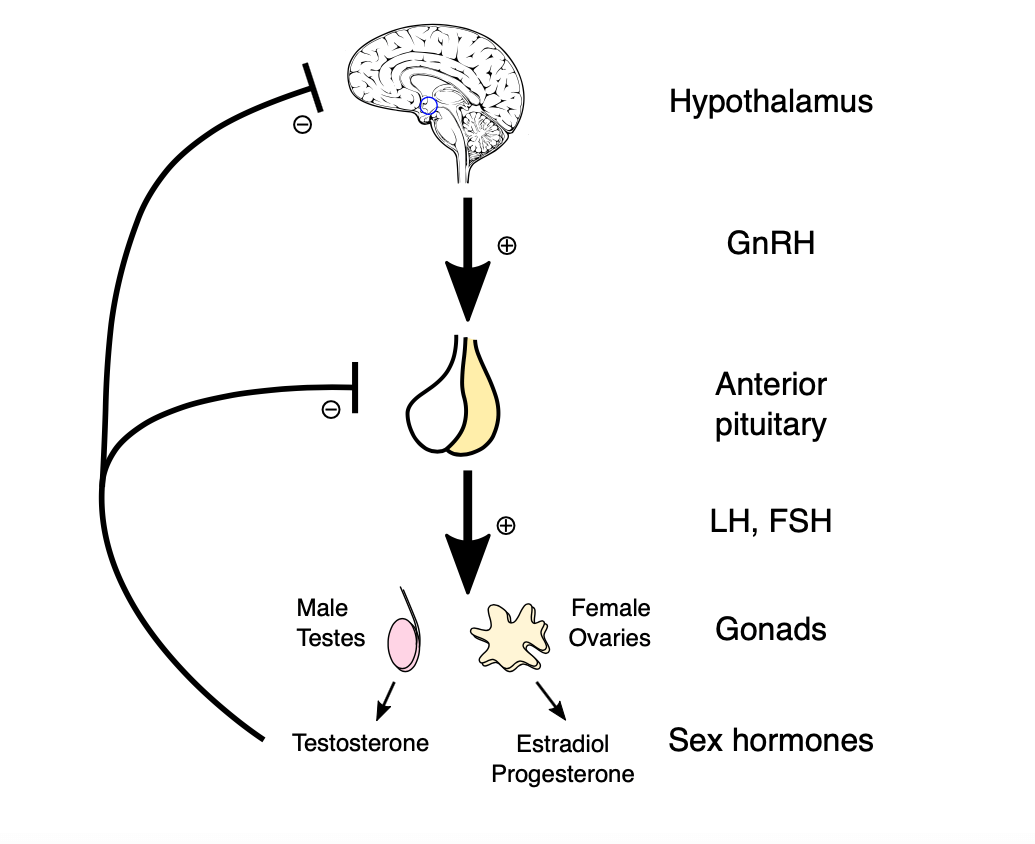
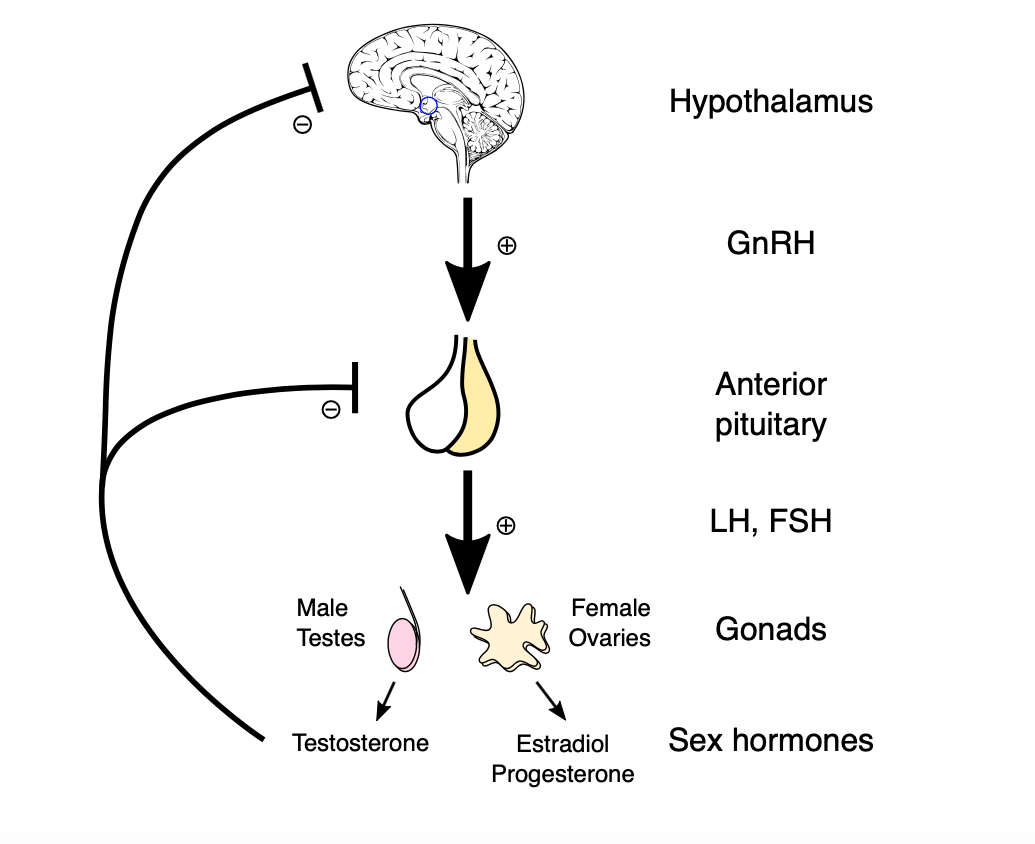
The onset of puberty is governed by a sophisticated endocrinological orchestra primarily involving the hypothalamic-pituitary-gonadal (HPG) axis. The hypothalamus secretes gonadotropin-releasing hormone (GnRH), stimulating the pituitary gland to release luteinizing hormone (LH) and follicle-stimulating hormone (FSH). These hormones catalyze sexual maturation, resulting in the production of sex steroids such as testosterone and estrogen. These biochemical agents trigger the phenotypical changes recognized as puberty, including growth spurts, secondary sexual characteristics, and alterations in brain architecture.
In neurotypical adolescents, these changes tend to follow a somewhat predictable trajectory; however, for those with autism spectrum disorder (ASD), the hormonal variability can exacerbate or modulate existing neurobehavioral profiles. The bidirectional influence between hormones and the autistic brain necessitates a deeper exploration into how puberty unfolds uniquely within this population.
Behavioral and Emotional Shifts During Puberty in Autism
As puberty progresses, autistic adolescents may experience amplified challenges in emotional regulation, social interaction, and sensory processing. The hormonal surges associated with puberty can exacerbate mood instability, leading to heightened anxiety, irritability, and instances of emotional dysregulation. This volatility often overlaps with the core features of autism, such as difficulties with communication and social reciprocity, creating a compounded effect that can be difficult to navigate.
Moreover, sensory sensitivities frequently intensify. Hormonal flux can alter sensory thresholds, making stimuli that were once tolerable become overwhelming. This can manifest as increased avoidance behaviors, meltdowns, or withdrawal, which further complicate social integration and academic engagement.
Pubertal Development and Physical Health Considerations
Beyond behavioral ramifications, pubertal physical changes pose distinct considerations for autistic individuals. Growth spurts, acne, voice changes, and menstruation may provoke confusion or distress, especially if communication deficits hinder expressive description of bodily changes. Additionally, autistic youth may exhibit atypical responses to these bodily transformations, including aversion to hygiene routines or altered proprioceptive feedback.
Medical monitoring becomes paramount. Health care providers must adopt a vigilant, individualized approach that respects sensory preferences and communication styles while ensuring that routine screenings and interventions related to puberty are effectively managed. Collaboration across disciplines, including endocrinology, psychiatry, and occupational therapy, can facilitate holistic care.

The Influence of Hormonal Changes on Autism-Specific Behaviors
Puberty may introduce an inflection point for the manifestation of autistic traits. For instance, repetitive behaviors and restricted interests, hallmark features of autism, can either intensify or diminish depending on how hormonal shifts impact neurological circuits. Some adolescents report a surge in obsessions or routines as a form of coping mechanism amid the unpredictable internal environment.
In addition, social cognition—already a challenging domain—faces added pressures. The maturation of brain regions involved in theory of mind and emotional recognition occurs alongside hormonal changes, sometimes revealing new dimensions in social difficulties. Conversely, some individuals may experience gains in abstract reasoning or self-awareness that can facilitate greater self-advocacy and adaptive strategies.
Gender Differences and Puberty in Autism
Gender-specific hormonal changes introduce further complexity. Autistic girls may confront unique challenges associated with menstruation, including irregular cycles, premenstrual syndrome (PMS), and menstrual hygiene management difficulties, which can be compounded by sensory sensitivities. These factors often contribute to increased anxiety or mood disturbances.
Conversely, autistic boys undergoing surges in testosterone might exhibit intensified aggression, impulsivity, or mood lability. These behavioral changes can lead to misunderstandings or punitive responses unless caregivers and educators are equipped with an informed perspective and adaptive strategies.
Recognizing these gender-based distinctions is critical to tailoring clinical assessments and interventions. Gender-sensitive support frameworks can empower individuals during puberty to navigate biological and social changes more effectively.
Supporting Autistic Individuals Through Adolescence and Beyond
Transitioning through puberty and into adulthood represents a pivotal period for fostering autonomy, resilience, and well-being. Support systems must evolve to meet the emerging needs associated with hormonal maturation while respecting the nuances of autism. Psychoeducation for families, educators, and clinicians is indispensable, ensuring that emotional and physiological changes are anticipated and managed constructively.
Therapeutic modalities such as cognitive-behavioral therapy (CBT), sensory integration therapy, and social skills training can be optimized to acknowledge pubertal impacts. Adaptive approaches that incorporate flexibility, routine, and individualized learning are most effective in promoting positive outcomes.
Moreover, hormone-related medical concerns must be vigilantly addressed, such as managing menstrual pain, acne treatments, or addressing potential hormonal imbalances. Regular collaboration between neurologists, endocrinologists, and mental health specialists provides a comprehensive care model that fosters holistic development.

Ultimately, understanding and supporting autistic individuals through puberty and beyond requires a multifaceted lens that embraces biological, psychological, and social dimensions. Acknowledging the distinctive pathways of development within this population enhances compassion, enhances care, and lays the foundation for healthier transitions into adulthood.